Quadriceps-sparing total knee replacement is a contemporary approach to knee arthroplasty that preserves the quadriceps tendon and limits trauma to surrounding soft tissues. By avoiding a large incision through the quadriceps tendon, this technique is intended to support early mobility, reduced postoperative pain, and help patients resume daily activities sooner. Below, learn how the procedure works, how it compares with traditional methods, the Jiffy Knee approach, and who may be a good candidate. For patients searching for the latest in knee replacement surgery, the quad sparing total knee replacement technique is a thoughtful, evidence-informed choice that our team carefully considers for each individual.
Quadriceps-Sparing Total Knee Replacement: What to Know
What Is Quadriceps-Sparing Total Knee Replacement?
This procedure replaces damaged joint surfaces in the knee while maintaining the integrity of the quadriceps tendon and extensor mechanism. Surgeons work around the tendon rather than through it, navigating between natural tissue planes to access the joint and accurately position implants. In plain terms, if you have wondered, “are muscles cut during knee replacement surgery?” the goal with a quad sparing knee replacement is to avoid cutting the quadriceps tendon and minimize disruption of surrounding muscle fibers whenever safely possible.
The technique evolved from approaches developed in the early 1990s.1 As specialized instruments and imaging guidance improved, surgeons refined methods to avoid splitting the quadriceps tendon without compromising implant alignment or stability. It is commonly used to treat severe osteoarthritis and other advanced degenerative conditions that cause pain, stiffness, and loss of function when non-surgical measures are no longer effective. Among the types of knee replacement available today, quad sparing total knee replacement is considered part of the latest in knee replacement surgery, focused on soft tissue preservation and early function.2
Benefits of a Quadriceps-Sparing Approach
- Faster early recovery: Preserving the quadriceps tendon can facilitate earlier straight-leg raises, walking, and stair climbing.3
- Less muscle disruption: Protecting the extensor mechanism may help maintain strength and knee control, supporting a more efficient rehabilitation process and a quicker return to a normal gait. Patients often ask, “are tendons and ligaments cut during knee replacement?” With a quadriceps-sparing technique, the aim is to protect the entire quadriceps mechanism to reduce postop dysfunction.4
- Reduced early pain and swelling: Limiting soft tissue trauma often improves comfort in the first weeks after surgery and may reduce the need for inpatient rehabilitation.3,5
All surgical procedures carry risks such as infection, blood clots, stiffness, implant loosening, and anesthesia-related issues. Careful surgical technique, multimodal pain control, and early mobilization help mitigate many of these risks. Long-term outcomes with quadriceps-sparing techniques are comparable to traditional approaches when performed by experienced surgeons. If you have concerns about “how are muscles reattached after knee replacement,” rest assured that when muscle or tendon detachment is required in other approaches, surgeons use robust suture techniques to reattach and protect healing; with quad sparing knee replacement, the intention is to avoid muscle separation in the first place.
How It Differs From Traditional Knee Replacement
Surgical exposure: Traditional total knee replacement often uses a midline incision with a split in the quadriceps tendon separating the vastus medialis from remaining three quadriceps muscles to access the joint. Quadriceps-sparing techniques use a muscle sparing approach to avoid cutting the tendon, preserving the extensor mechanism. This directly addresses concerns such as “are muscles cut during knee replacement surgery,” as the quad sparing total knee replacement approach is designed to minimize that need.
Rehabilitation and function: Because the tendon remains intact, patients can typically begin active knee extension earlier. Many experience less early pain and greater confidence with movement, which can translate into smoother physical therapy sessions and faster achievement of mobility milestones.2,3,4,5
Outcomes: Early recovery measures—pain, range of motion, and function—have been shown to be improved with quadriceps-sparing methods. Long-term implant performance and overall function are similar to traditional techniques when alignment and soft tissue balancing are precise around 1 year postoperatively. For those asking “how are muscles reattached after knee replacement,” traditional methods may require tendon repair; quadriceps-sparing methods are designed to avoid that step while maintaining accuracy.
Quadriceps-Sparing vs. Jiffy Knee
Jiffy Knee is a branded, muscle-sparing total knee replacement approach that emphasizes limited disruption to the quadriceps and surrounding soft tissues. Both quadriceps-sparing and Jiffy Knee aim to reduce early pain and speed recovery by protecting the extensor mechanism through the same medial subvastus approach to the joint. Patients comparing a quad sparing knee replacement to a jiffy knee replacement will find overlapping principles focused on soft tissue preservation.
| Feature | Quadriceps-Sparing TKA | Jiffy Knee |
|---|---|---|
CORE PRINCIPLE | Avoids incising the quadriceps tendon; uses tissue planes to access the joint | Branded muscle-sparing technique with similar tendon-preserving goals |
INCISION AND EXPOSURE | Medial subvastus muscle sparing approach; standard instruments or specialized tools | Proprietary instruments and protocols may be used through the same medial approach and a more medial incision |
RECOVERY FOCUS | Earlier straight-leg raises, walking, and confidence with movement | Marketed for rapid recovery with early function and reduced pain |
OUTCOMES | Early advantages with comparable long-term results to traditional TKA | Similar expectations: outcomes depend on surgeon expertise and implant alignment |
In practice, the similarities are greater than the differences. Both rely on the concept of a muscle sparing approach to the knee, careful soft tissue handling, and precise implant positioning. The best choice is often the technique your surgeon performs most frequently and effectively, tailored to your knee anatomy and goals. When considering what technique might suit your knee replacement best, our guidance remains individualized and focused on safety and function.
Who Is a Good Candidate?
- Advanced knee osteoarthritis or other degenerative conditions causing significant pain and mobility limitations despite non-surgical care
- Favorable soft tissue quality and alignment that allow adequate exposure without cutting the quadriceps tendon
- Realistic expectations and willingness to participate in a structured rehabilitation program
Both younger, active adults and older patients can be candidates. Suitability depends more on joint damage, bone quality, and overall medical fitness than age alone. Active individuals may appreciate faster early recovery, while older adults may benefit from reduced pain and earlier independence. Not every knee is appropriate for a quadriceps-sparing or jiffy knee replacement approach; some patterns of deformity or prior surgery may necessitate alternative types of approach to knee replacement.
The evaluation typically includes a full medical history, physical examination, weight-bearing X-rays, and sometimes advanced imaging. If you have questions like “are tendons and ligaments cut during knee replacement,” we will explain how quadriceps-sparing techniques aim to preserve these structures while still achieving proper alignment and stability.
What to Expect
Most patients begin walking with assistance the day of their surgery and start physical therapy focused on range of motion, swelling control, and progressive strengthening within a week. Many can perform basic daily activities within a few weeks, though full recovery varies based on individual factors and adherence to rehabilitation. Your care team will provide guidance on wound care, medications, activity progression, and long-term joint protection. As part of the latest in knee replacement surgery, our protocols emphasize comfort, safety, and steady progress.
If you are considering knee replacement and want to know whether a quadriceps-sparing total knee replacement is right for you, schedule a consultation with Dr. D. Alex Forrester, who specializes in quadriceps-sparing knee replacements. A personalized assessment can help determine the safest technique that aligns with your anatomy, goals, and lifestyle—whether that is a quad sparing total knee replacement or another evidence-based option among the types of knee replacement we offer.
References:
- Hofmann, A.A. ∙ Plaster, R.L. ∙ Murdock, L.E. Subvastus (southern) approach for primary total knee arthroplasty. Clin Orthop Relat Res.1991; 70-77
- Stubnya B, Kocsis K, Váncsa S. Subvastus Approach Supporting Fast-Track Total Knee Arthroplasty Over the Medial Parapatellar Approach: A Systematic Review and Network Meta-Analysis. Journal of Arthroplasty, 2023; 38, 2750-2758
- Roysam GS, Oakley MJ. The Subvastus Approach for Total Knee Arthroplasty Resulted in Better Short-Term Outcomes than Did the Parapatellar Approach. A prospective, randomized, and observer-blinded trial. J Arthroplasty. 2001;16:454–457. doi: 10.1054/arth.2001.22388.
- Chang CH, Chen KH, Yang RS, Liu TK. Muscle torques in total knee arthroplasty with subvastus and parapatellar approaches. Clin Orthop Relat Res. 2002;98:189–195. doi: 10.1097/00003086-200205000-00027
- Sastre S, Sanchez MD, Lozano L, Orient F, Fontg F, Nun˜ez M. Total knee arthroplasty: better short-term results after subvastus Approach. A Randomized, controlled study Knee. Surg Sports Traumatol Arthrosc. 2009;17:1184–1188. doi: 10.1007/s00167-009-0780-6.
The Link Between BMI and Joint Health: How Weight Impacts Hip and Knee Joint Longevity
As we’ve heard many times before, maintaining a healthy body weight is crucial for overall health, however the impact of a healthy body weight on specific body parts, specifically the hip and knee joints, is often underestimated. Body Mass Index (BMI), a measure of body fat based on height and weight, along with the measure of relative muscle mass, can significantly affect the health and longevity of these weight-bearing joints. Today, we’ll discuss the correlation between BMI and joint health, with focus on the hip and knee joints, and how weight management plays a crucial role in preserving joint function and longevity.
It is important to note, muscle mass has a great influence on BMI measurements as BMI is factored upon height and weight and does not differentiate between muscle mass and fat mass. Muscle tissue is denser than fat tissue, therefore a person with a high muscle mass, but relatively low fat mass may have a higher weight resulting in a higher BMI measurement. This does not necessarily mean that the individual is overweight or unhealthy. The impact of BMI on weight-bearing Joint Longevity discussed within this article, does not pertain to those of high muscle mass with low fat mass measurements.
The Impact of BMI on Hip Joints
The hip joint is one of the largest weight-bearing joints in the body and is responsible for supporting our body weight during both sedentary activities and when facilitating movement. Studies have shown that a higher BMI is associated with an increased risk of hip osteoarthritis, a degenerative joint disease characterized by the breakdown of cartilage and bone within the joint. This is because the excess body weight places additional stress on the hip joint, accelerating the wear and tear process and increasing the risk of developing osteoarthritis. Maintaining a healthy BMI through a nutrient dense diet and consistent exercise regimen can help preserve joint function and longevity.
The Effect of BMI on Knee Joints
Similar to the hip joint, the knee joint is also susceptible to the effects of excess body weight. Studies have demonstrated a clear link between higher BMI and an increased risk of knee osteoarthritis. The excess weight puts pressure on the knee joint, leading to cartilage damage and inflammation, which are key indicators of osteoarthritis onset. Additionally, higher BMI is associated with an increased risk of knee injuries, such as tears in the ligaments or meniscus, further compromising joint health. By maintaining a healthy BMI, individuals can help protect the integrity of their knee joints, reducing the risk of developing knee osteoarthritis and either delaying the need for a total joint replacement or avoiding one altogether.
The Role of Weight Management in Joint Health
Weight management plays a crucial role in preserving the longevity of the hip and knee joints. For individuals who are overweight or obese, losing even a modest amount of weight can significantly improve joint function.
Maintaining a healthy weight and BMI measurement is especially crucial when looking to qualify for a total joint replacement as BMI is one of the several factors considered when determining a patient’s eligibility for a hip replacement or knee replacement. Although there is not a specific BMI ‘cutoff’ that qualifies or disqualifies a patient, risks such as infections, blood clots, and anesthesia complications, exponentially increase in those with higher BMIs. Generally, a BMI below 40 is preferred as qualification for a total joint replacement to reduce these risks.
The decision to move forward with a hip or knee replacement surgery is inevitably up to the individual and their orthopedic specialist who will complete a comprehensive evaluation of the patient’s overall health, the severity of joint damage, pain during daily activities, and functional limitations. If recommended to reduce one’s BMI measurement, a combination of regular physical activity, such as low-impact exercises like swimming or cycling, or resistance training combined with a nutrient dense diet can help individuals achieve and maintain a healthy BMI, reducing the burden on their joints and maintaining joint health for the long run.
To schedule an appointment with one of our Board Certified and Fellowship Trained specialists, give us a call at 719-632-7669 or visit us at www.CSOG.net to learn more.
Anterior Hip Arthroplasty, Advancing Hip Replacement Outcomes and Longevity
Hip replacement surgery has come a long way since its inception with new techniques continuously evolving to improve outcomes, patient satisfaction, and implant longevity. One such advancement is the use of the anterior approach hip replacement surgery, a technique that differs from traditional approaches (posterior and lateral) and offers many unique benefits. Today, we’ll delve into:
– What Anterior Hip Replacements are
– The History of Anterior Hip Replacements
– How they differ from other techniques
– What recovery generally looks like
– Candidacy for this innovative procedure
What are Anterior Hip Replacements?
Anterior hip replacement surgery is a minimally invasive surgical technique used to replace a damaged hip joint with an artificial implant. Unlike traditional hip replacement surgeries that access the hip joint from the side or back (lateral or posterior approaches), the anterior approach accesses the joint from the front (anterior aspect) of the hip, through a small incision.
A Brief History
While the anterior approach to hip replacement is often considered a modern innovation, its roots can be traced back to the early 20th century. Dr. Marius Smith-Petersen, an American orthopedic surgeon, first discussed the anterior approach in the 1940s. However, it was not widely adopted due to technological challenges and the popularity of other approaches. The first anterior hip replacement surgery was performed in 1947. It wasn’t until the late 20th and early 21st centuries that advancements in surgical techniques, imaging technology, and implant design made anterior hip replacement a more feasible option. Since these advancements, the procedure has gained immense popularity among surgeons and patients alike.
How Anterior Hip Replacement Differs
The anterior approach offers several advantages over traditional lateral and posterior approach hip replacement techniques including:
- Muscle Preservation: One of the key benefits of the anterior approach is that it allows access to the hip joint without detaching muscles from the pelvis or femur. A muscle-sparing technique such as this, can lead to faster recovery times and in many cases, less postoperative pain compared to other techniques..
- Stability: Thanks to this muscle preservation, the anterior approach shows an increased stability of the implant due to the preservation of the surrounding soft tissues and muscles. This added stability can reduce the risk of dislocation.
- Additional Accuracy: The anterior approach provides excellent visualization of the hip joint, allowing for even more precise placement of the implant during surgery.
- Faster Recovery: Patients who undergo anterior hip replacement surgery may experience a quicker recovery compared to other techniques. This is primarily due to the muscle preservation benefits, which can lead to less damage to the surrounding structures and a faster return to normal activities.
Video credit to Stryker Orthopedics
Anterior Hip Replacement Recovery
Studies show recovery from Anterior Approach Hip Replacement Surgery enables the potential for early mobility. One of the primary advantages of the anterior approach is that it typically allows for early mobility. Patients may be able to walk with a cane or walker soon after surgery, often times within a couple hours of surgery. This is due to the muscle preservation nature of the approach, again, leading to less damage to the surrounding structures and a faster return to normal activities.
While hip precautions are often recommended for all types of hip replacement surgeries to prevent dislocation of the new hip joint, the specific precautions may vary depending on the surgical approach. For example, patients undergoing an anterior approach may be advised to avoid certain movements that could strain the front of the hip joint especially within the initial recovery period.
Rehabilitation following an anterior approach hip replacement surgery typically focuses on restoring range of motion, strength, and function. To kickstart the recovery process, Physical therapy begins soon after surgery to help patients regain mobility and strength in the hip joint and return to normal activities, including driving, quickly and efficiently.
It’s important to note that the recovery process can vary from patient to patient due to individual factors regardless of the surgical approach. Factors such as age, overall health, and the extent of joint damage can all impact the recovery timelines and overall outcome. Patients should follow their surgeon’s postoperative instructions and participate in any rehabilitation programs as prescribed to optimize their recovery.
Who Would Be a Candidate?
While anterior hip replacement surgery offers many benefits, not everyone is a candidate for this procedure. Ideal candidates for anterior hip replacement surgery typically include those who are:
- Physically Active: Patients who are physically active and in good overall health may benefit from the faster recovery times associated with the anterior approach.
- Of Healthy BMI: Patients who are within a healthy BMI generally have better outcomes with the anterior approach, as excess body weight can put additional stress on the hip joint and may impose greater risk of complications during and after surgery. Tune into our blog discussing The Link between BMI and Joint Health
- Motivated Patients: Patients who are motivated to actively participate in their recovery process, including following postoperative rehabilitation protocols, achieve better results with the anterior approach.
Candidacy for any hip replacement technique ultimately comes down to what is best for the individual patient and their lifestyle as discussed with their orthopedic specialist.
In conclusion, Anterior Hip Arthroplasty surgery is a modern hip replacement technique that offers several advantages. With its muscle preserving technique, increased stability, and faster recovery times, it has become an attractive option for many surgeons and patients seeking hip replacement surgery with hopes of returning to activities.
If you’d like to discuss your candidacy for an anterior hip replacement, give us a call at 719-632-7669 to schedule with one of our board certified Joint Replacement specialists.
The Fellowship Trained and Board Certified Difference
When it comes to Orthopaedic care, choosing the right physician is crucial for ensuring optimal treatment and recovery outcomes.
Amongst Orthopaedic physicians, there are different levels of training and certifications. Each can significantly impact their level of expertise and capacity for providing the full spectrum of comprehensive care. When looking at a physician’s bio, especially those that are apart of the team here at CSOG, you’ve likely seen the terms: fellowship trained and board certified. But what do these terms actually mean? What type of training has the physician gone through to receive these credentials?
Fellowship Training:
Specialization and Expertise
What does fellowship trained mean? Fellowship training is an additional period of intensive, specialized training that orthopaedic surgeons pursue after completing their residency program. During this fellowship, physicians focus on a specific area within orthopaedic surgery, such as sports medicine, joint replacement, spine surgery, foot and ankle surgery, or hand and upper extremity surgery, among others. These fellowship programs require physicians to participate in hundreds of specialized surgeries to develop advanced skills and expertise in their chosen subspecialty before they’re eligible to receive the fellowship trained credential.
Benefits of Fellowship Training
- Enhanced Knowledge and Skill Set: Fellowship-trained orthopaedic physicians possess a deeper understanding of their specific area of focus due to their additional, rigorous training that allowed them to gain extensive hands-on experience from leaders within the orthopedic world. This experience enables them to address complex cases and provide highly specialized, individualized care.
- Leaders of Orthopedic Advancements: Fellowships provide consistent access to the latest research, techniques, and technologies in the specific subspecialty. Not only does this exposure keep physicians abreast of recent advancements, it allows them to continue development upon such innovation to ensure patients receive the most effective and lasting treatment options.
- Collaboration and Networking: Fellowship programs often foster collaboration and networking among specialists, enabling physicians to consult with colleagues and share knowledge across the nation. This collaborative environment further enriches their expertise and promotes the exchange of best practices.
Board Certification:
Recognized Expertise and Quality Assurance
What does Board Certified mean? Board certification is a rigorous process that evaluates a physician’s knowledge, skills, and clinical experience in a particular medical specialty. To become board certified, orthopaedic surgeons must complete a specific number of postgraduate training years. Then, they are eligible to complete a comprehensive oral and written examination administered by the American Board of Orthopaedic Surgery (ABOS) or an equivalent board such as the American Osteopathic Association (AOA) for Doctor of Osteopathic Medicine (DOs).
Importance of Board Certification
- Expertise Verification: Board certification serves as an independent
 validation of an orthopaedic surgeon’s knowledge and expertise in their specialty and demonstrates that the physician has met the meticulous standards set by the ABOS or the equivalent certifying body.
validation of an orthopaedic surgeon’s knowledge and expertise in their specialty and demonstrates that the physician has met the meticulous standards set by the ABOS or the equivalent certifying body. - Commitment to Continuous Learning: Maintaining board ce
rtification requires ongoing professional development through continuing medical education (CME) credits. These CME requirements ensure that certified physicians stay current with advancements in their field and provide patients with the most up-to-date care. - Quality Assurance: Board certification acts as a quality assurance measure for patients, as it signifies that the orthopaedic physician meets or exceeds the established standards of practice.
The Doctor’s Timeline
Becoming a physician is no easy feat. Especially one with high distinctions of Fellowship Training and Board Certification. On average, in addition to completing a four-year undergraduate degree, a physician must complete four years of medical school. After medical school, they will complete a five-year residency program. Orthopedists such as ours within CSOG, then apply for a fellowship program. Only the best candidates are granted participating into these fellowships that typically last an additional year. To become board certified, the physician must meet their respective board’s mandated training hours. Depending on the board, this can take between 3-7 years. Added together, a fellowship trained and board-certified Orthopaedic physician has undergone anywhere between 17-21 years of training and education.
With their Fellowship training and the addition of a Board certification, physicians are focused extensively on specific subspecialties, with the advanced skills necessary to ensure high quality outcomes backed with quality assurance to their commitment of providing high-quality care. In the realm of orthopaedic care, patients can rest assured they’re in qualified hands when seeking specialized or complex treatments through fellowship-trained and board-certified orthopaedic physicians.
What is Osteoporosis?
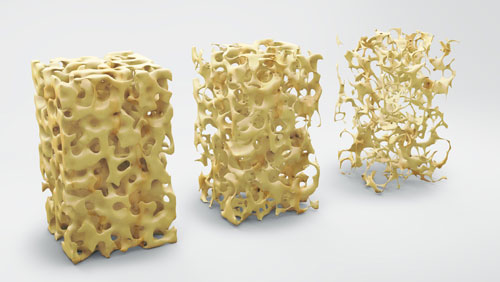
Osteoporosis is a disease that occurs when bone density and/or the quality of your bone decreases, causing weak bones. It occurs when the density and quality of bone are reduced. Normally, bones go through a process called “Remodeling” where old bone is broken down and new bone is built in its place. However, in osteoporosis, the creation of new bone is unable to keep pace with the removal of old bone, resulting in a net loss of bone mass.
Who is at risk for Osteoporosis?
There are several clinic risk factors that can contribute to the development of osteoporosis including:
- Age: Around the age of 40, the bone building part of the remodeling process begins to slow down which results in a net loss over time. This imbalance becomes even more prevalent after menopause.
- Gender: Women are more likely to develop osteoporosis than men due to hormonal changes during menopause.
- Genetics: A family history of osteoporosis can increase the risk.
- Hormonal changes: Low estrogen levels in women and low testosterone levels in men can lead to bone loss.
- Unhealthy Lifestyle Habits and Vitamin Deficiencies: Lack of physical activity, a diet poor in calcium and vitamin D, smoking, excessive alcohol consumption, and certain medications can all contribute to bone loss.
- Medical Conditions: Some medical conditions, such as celiac disease, rheumatoid arthritis, and hormonal disorders, can increase the risk of osteoporosis.
- Medications: Long-term use of certain medications, such as corticosteroids and some anticonvulsants, can weaken bones.
Each of these, especially when compounded, can ultimately result in a fracture or at minimum, an increased risk of fracture which can occur even with minor trauma or stress on the bones. The most common sites of an osteoporotic fracture are wrists, hip, and spine. Fractures, particularity those of the hip, have potential for serious consequences for older adults and can lead to decreased mobility and independence.
How is Osteoporosis Prevented and Managed?
Preventing and managing osteoporosis typically involves lifestyle changes including adopting a nutrient dense diet and vitamin regimen, regular weight-bearing exercise, smoking cessation, alcohol moderation, and possible medication management. It is important to know this is a lifelong diagnosis with several possible treatment pathways that are individualized to each patient. A detailed interview along with imaging and labs will help determine treatment recommendations.
Regular bone density testing can help diagnose osteoporosis early and help guide the treatment process as well. Early detection and proactive management are essential in reducing the risk on further onset and the risk of potential fractures.
What is Bone Density?
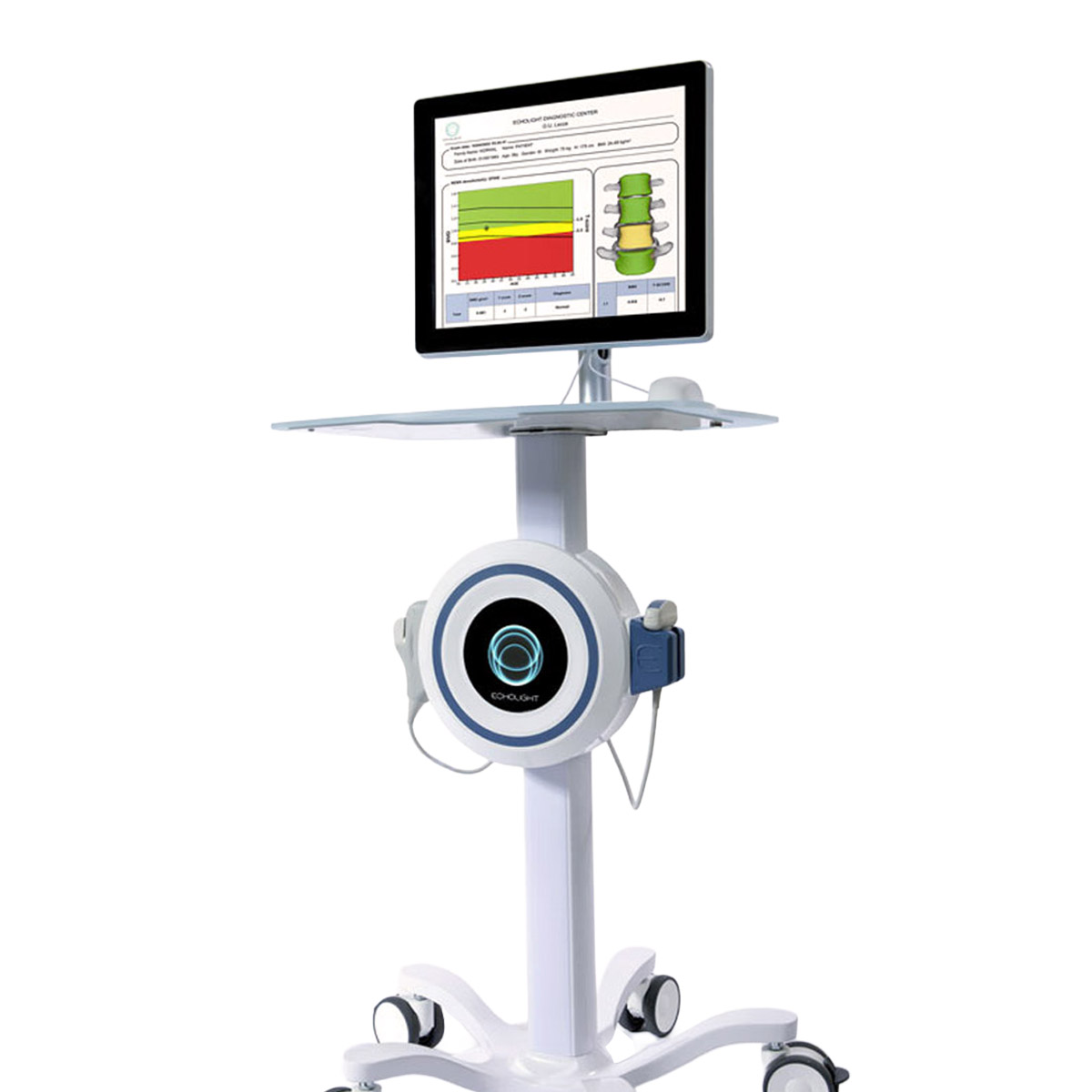
Bones density, also known as Bone Mineral Density, is the total amount of bone mineral within boney tissue. Bone Density is measured using low-dose x-ray tests called DEXA or DXA scans that measure calcium and additional minerals within the bones. This measurement helps determine the strength and thickness (density) of bone which then helps providers predict a patient’s fracture risk.
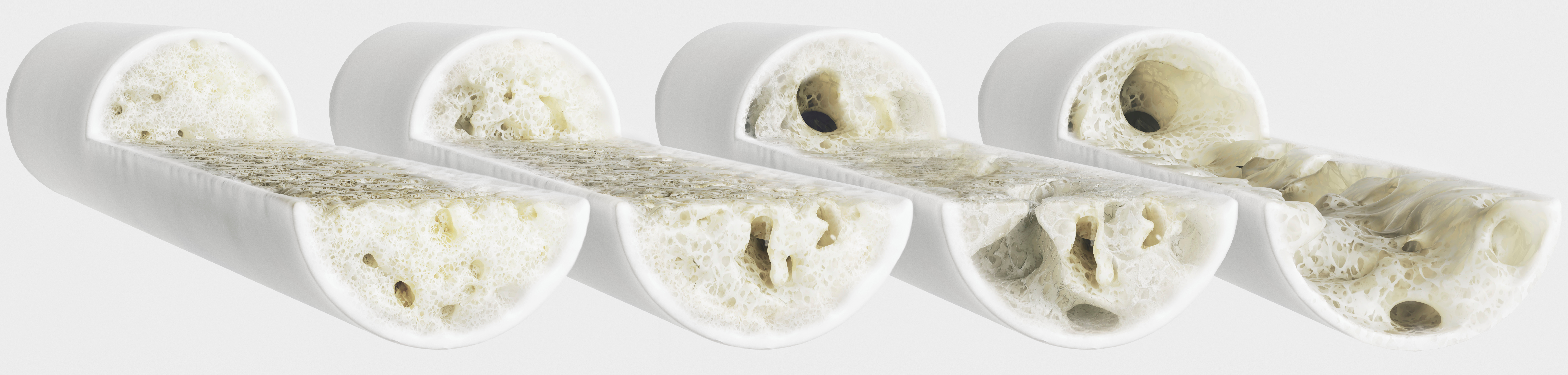
Stay tuned as we continue our Bone Health series and further discuss treatment methods, FRAX scores, and much more.
Healing Connection
Healing Connection with Eric Jepson, DO
with Eric Jepson, DO , written by Alyssa Shikles of Colorado Springs Magazine. Photography by: Meegan Dobson
It takes a skilled doctor to ease a worried patient’s mind. After all, no one visits the doctor for fun. You go because something’s wrong or because you’re afraid something’s wrong. You’re looking for hope in the midst of pain, for answers when your own body feels unknown and uncertain. In these moments of stress and anxiety, a good doctor—with a comforting word and a desire to meet patients where they are—can have an incredible emotional and physical impact.
For Eric Jepson, MD, an orthopedic surgeon at Colorado Springs Orthopedic Group (CSOG), this is the most critical and challenging facet of his job. For him, fixing the body is easy; the hard part is gaining trust and making patients feel cared for.
When I sat down to talk with Dr. Jepson in CSOG’s south office a few weeks ago, I experienced first-hand how relational he is. There’s something about him that exudes not only kindness and understanding but relatability and genuine interest in others. He has a keen listening ear, and though I came to his office to interview him, I was surprised when he often flipped questions back on me. How long have I lived in Colorado Springs? Do I love the outdoors? How did I handle my first Colorado winter? He wanted to get to know me, and I felt seen.
This small interaction is just a sampling of how Dr. Jepson interacts with patients daily. But to him, making patients comfortable and being present for them is fundamental to his day-to-day work. Anyone can work with a scalpel or heal a wound if they study hard enough, but learning to connect with others relationally? That’s what makes a stand-out physician.
Total Knee Replacement vs Partial Knee Replacement
Total Knee Replacement vs Partial Knee Replacement
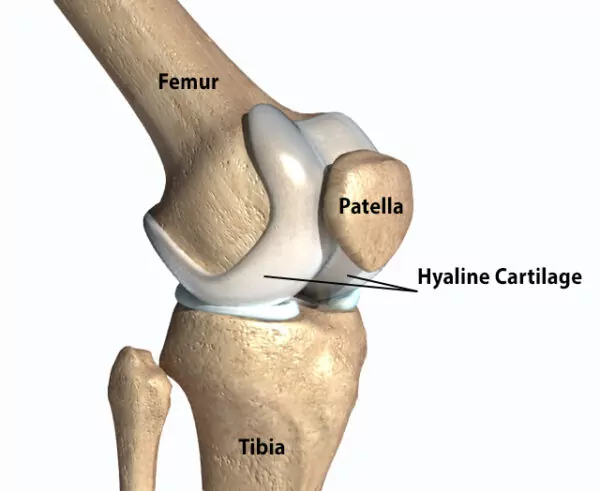
Joint Replacement surgeries, specifically Knee Replacement surgeries, have become some of the most common procedures performed across the globe. This is due to many types of arthritis affecting our joints and causing joint damage. Much like the end of a chicken bone, our bones are covered with a thin but resilient layer called Hyaline Cartilage. Arthritis can be thought of as the progressive deterioration, or wear, of this layer. As this happens our underlying bones begin to rub against each other causing the substantial pain so many experience. These various types of arthritis can be caused from previous injuries, autoimmune conditions, or even simple wear and tear from activities and aging. Whatever the cause, the results can be debilitating.
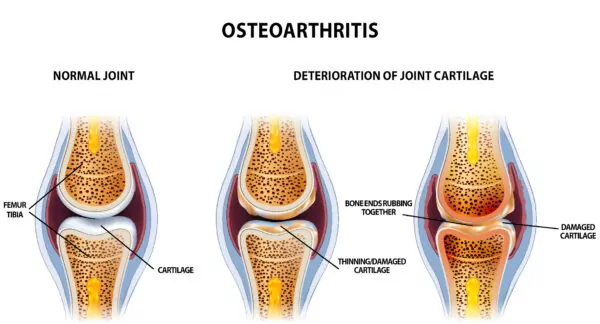
Symptoms of Arthritis
Symptoms of Arthritis range from mild stiffness and soreness to the loss of proper anatomical (muscular and skeletal) function, severe pain consistently felt within the joint, and the inability to walk. As a result, many ask when is it time to see a doctor to seek pain relief for arthritis? In short, if the pain is keeping you from performing your day-to-day activities, we recommend scheduling with a fellowship trained orthopedic joint specialist to see what treatment options will suit your individual symptoms and needs.
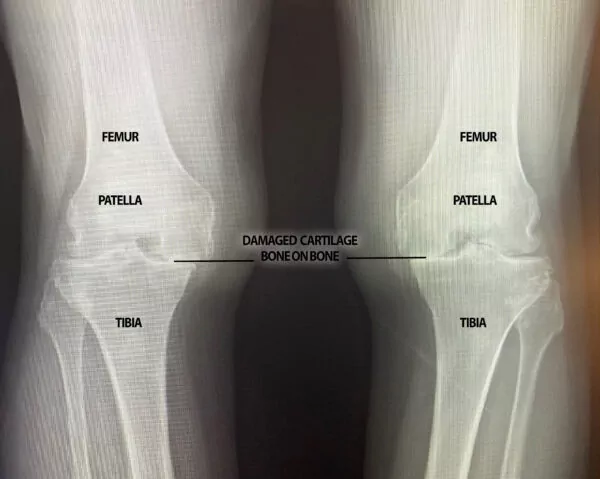
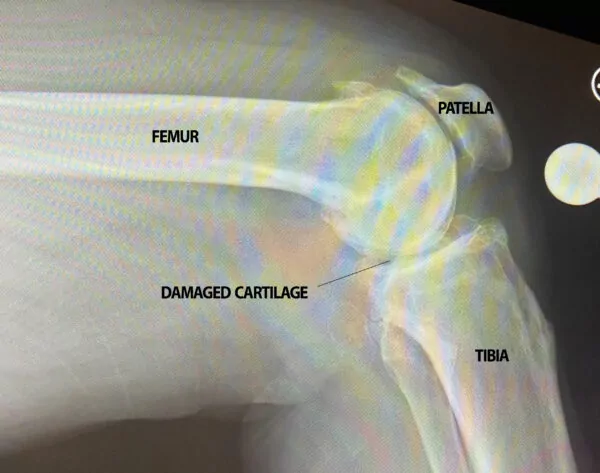
Treatment for Arthritis
For those who come to us with various symptoms of arthritis, there are a few initial steps that need to occur so we can appropriately diagnose your pain as arthritis pain and thus develop a suitable treatment plan for you.
The first step in diagnosis is taking you through a full examination of the joint in question and taking x-ray images. From here, you and your physician will work together to develop a treatment plan specific for the patients needs and lifestyle. In many cases, conservative treatments such as physical therapy or injection therapy, will be recommended as a starting point. If conservative treatment options are unable to help settle the arthritis pain, surgery is often our next best option.
Over the years, the surgeries used to treat arthritis pain have become very commonplace, exceptionally reliable, and tremendously rewarding for both the patient and surgeon when the patient returns to the activities they we’re limited from prior to treatment.
Total Knee Replacement vs Partial Knee Replacement
In most cases “Knee Replacement” can be thought of as a “Knee Resurfacing”. Essentially, the surgeon will remove the worn cartilage layer from the knee and replace (resurface) it with a new layer made of a very smooth hard metal and a medical-grade plastic to restore the joint.
Total Knee Replacement
In the knee, there are three main areas where our bones come in contact with each other. The femur, (thigh bone), the tibia (shin bone) and patella (kneecap). Restoring all three of these areas at one time is what we medically classify as a Total Knee Replacement. In many cases, by the time a patient comes to see us, their cartilage damage is severe enough, a Total Knee Replacement is the most appropriate treatment.
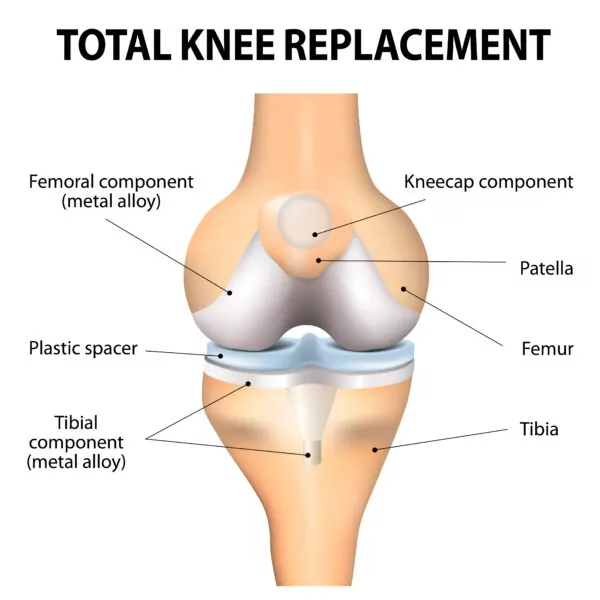
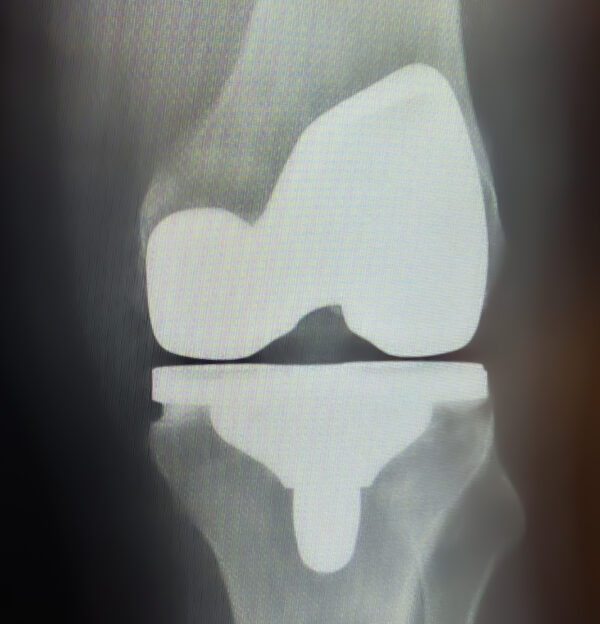
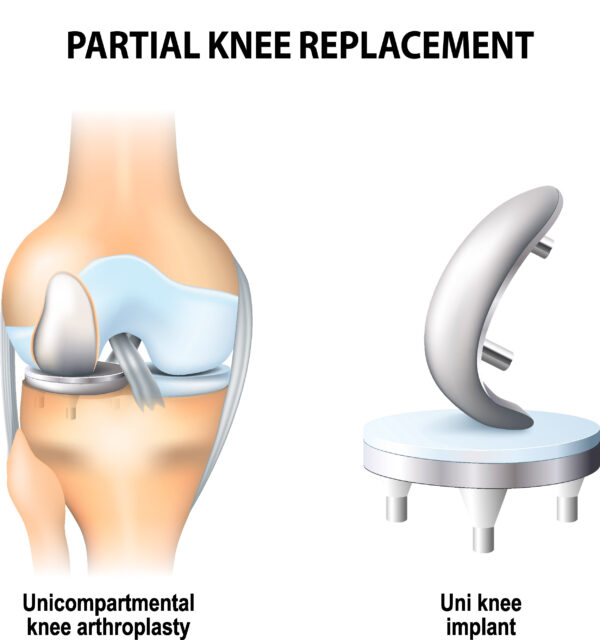
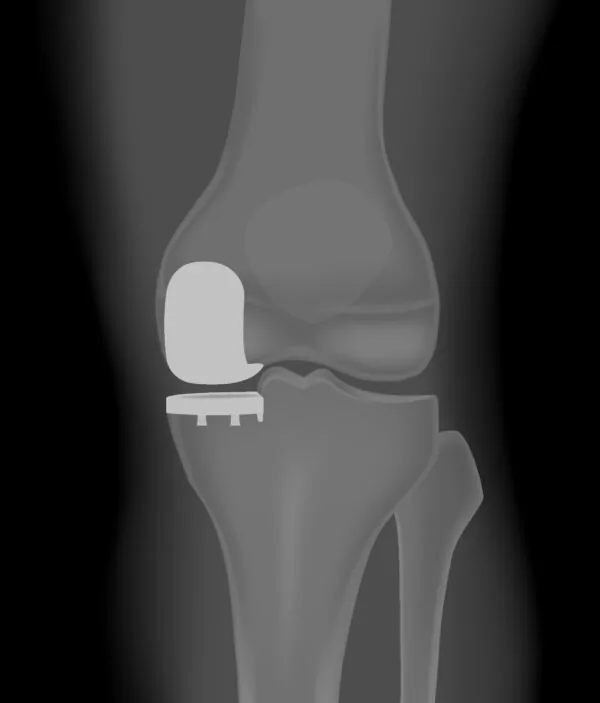
Partial Knee Replacement
Alternatively, there are some instances where only one of these three areas is the culprit for arthritis pain. In this case, a less invasive Partial Knee Replacement may sufficiently relieve the patient’s pain.
A Partial Knee Replacement procedure involves the removal of the one area of damaged cartilage and replacing it with a similar yet more localized hardware. The knee’s unaffected areas are left alone. With most cases, this procedure can be accomplished through smaller incisions causing less surgical injury to the knee. In other words, a Partial Knee Replacement could be classified as a minimally invasive surgery with less harm done to the knee compared to a Total Knee Replacement.
What to Expect with a Knee Replacement?
One thing to always remember, just because a procedure CAN be performed, does not mean it is always the correct choice. Always thoroughly discuss treatment options with your surgeon when making decisions to undergo surgery. To elaborate, there are some cases where you may not a good candidate for either one of these procedures. Your size, age, weight, overall health, outcome expectations, and physical limitations or abilities all play a role in whether a knee replacement will be the correct procedure for you. With this, no matter if a partial knee or a total knee replacement is chosen, the procedure must be able to:
- Be performed safely
- Improve your function
- Improve your quality of life
- Meet your physical ability expectations and support most tasks that you will place on it after surgery.
Furthermore, each procedure requires a visit to either a hospital or a surgery center, where the surgery is performed through an incision over the front of the knee. During the procedure you will be under anesthesia.
Keep in mind, a Total Knee Replacement and a Partial Knee Replacement will both involve some amount of downtime and commitment to a rehabilitation period after surgery. However, with technology advancements we are now able to have most patients up walking with assistance immediately after surgery. Additionally, in many cases we can perform the procedure as an outpatient procedure and send you home to recover the same day as surgery.
Knee Replacement Recovery Time
Although a partial knee replacement may be slightly less painful and overall an easier recovery than a total knee replacement, they are both very dependent on a strict and crucial rehabilitation period. The patient’s diligence with their postoperative physical therapy protocols is critically linked to the success of their surgery. Also, as mentioned previously, your preoperative condition and overall health status greatly affects success of the surgery as well as the time to reach full recovery. If post operative rehabilitation is adhered too, many patients are walking independently within days to weeks following the procedure. Likewise, some patients are able to go back to work within four to ten (4-10) weeks as well. After either type of knee replacement surgery, you can expect to see progressive improvement in your knee’s pain and function for up to a year.
If you are suffering from pain and stiffness in your knees that is not adequately controlled with a conservative treatment, talk with your orthopedic surgeon or call us today to schedule your initial evaluation.
Meet Our Providers
CSOG Comprehensive Joint Replacement Program Medical Minutes
CSOG Comprehensive Joint Replacement Program
Welcome to a Medical Minute segment with Dr. Tyler Bron, MD, Orthopedic Joint Replacement Surgeon as he introduces the New Comprehensive Joint Replacement Program at Colorado Springs Orthopedic Group.
Comprised of our four fellowship-trained Joint Replacement Surgeons and their teams, you can guarantee we will be with you every step of the way through your entire treatment journey! From initial consultation to post-operative rehabilitation, our clinical and case management teams will have you back on your feet as quickly as possible. When you become a patient of the Comprehensive Joint Replacement Program here at CSOG, you can expect a customized treatment plan designed specifically towards the severity of your condition using the most innovative and effective treatment methods available today.
Not only do our surgeons specialize in traditional joint replacements methods, they also specialize in minimally invasive surgical (MIS) techniques such as robotic assisted minimally invasive joint replacement procedures.
Outpatient total joint procedures performed in our ambulatory surgery center, The Orthopedic and Spine Center of Southern Colorado or within our community hospitals, allow the patient to recovery in the comfort of their own home the same day as surgery. Discuss with your physician if outpatient surgery is right for you as eligibility for these procedures may vary upon the severity of your injury or condition as well as your overall health.
CSOG has the largest group of fellowship-trained joint surgeons in southern Colorado and together have a combined 72 years of joint replacement experience. They pride themselves on the team approach, especially with severe cases our team of joint surgeons will meet and discuss in depth the most efficient treatment options to accelerate your recovery and get you back on your feet, doing the things you love to do, as quickly as possible.
To schedule your initial consultation, call us at 719-632-7669 today!
Visit www.CSOG.net to learn more.
Arthritis Types, Symptoms & Treatments with Dr. Tyler Bron
Arthritis Types, Symptoms & Treatments with Dr. Tyler Bron
Welcome to a Medical Minute segment with Dr. Tyler Bron, one of four fellowship-trained Orthopaedic physicians at Colorado Springs Orthopaedic Group. The video below will cover what arthritis is and discuss the different arthritis types, symptoms & treatments available at CSOG.
Arthritis Types: Osteoarthritis vs. Rheumatoid Arthritis
Arthritis comes in several different forms including Osteoarthritis and Rheumatoid arthritis. Osteoarthritis causes the cartilage, that lies between and protects the bones, to break down. Once this cartilage wears down, the bones become exposed to each other causing them to then rub against each other. This rubbing can cause inflammation and send pain signals to the brain. This is contrasted with Rheumatoid arthritis, which is caused by your body’s own immune system degrading the cartilage.
Who does Arthritis affect?
Arthritis can affect those of any gender or age, however, is most commonly seen when people get older. Arthritis, specifically Rheumatoid Arthritis, has a strong genetic component. Osteoarthritis is the most common form of arthritis and is known as “wear and tear arthritis” where previous joint injuries, overuse injuries, or obesity can be the primary cause.
Arthritis Symptoms
The most common symptoms of arthritis include an ache or dull pain that is constant and gets worse throughout the day depending on how active you are. As it progresses, the pain becomes more debilitating. Occasionally, arthritis progresses to the point where individuals are not able to live their desired active lifestyle. We recommend seeing an orthopedic specialist prior to this point.
Arthritis Treatment Options
There are non-surgical treatment options to treat arthritis. At Colorado Springs Orthopaedic Group, our physicians believe that in most cases, non-surgical treatment is the best place to start. Non-surgical interventions include weight loss, activity modification, avoiding high-impact sports activities, physical therapy, and the prescription of anti-inflammatory medications. Depending on the severity of your case, your physician may suggest a steroid injection that acts as an anti-inflammatory treatment. Once a patient has tried the above non-surgical options without experiencing long-lasting relief, then surgery may be a recommended option.
Colorado Springs Orthopaedic Group’s board-certified and fellowship-trained joint physicians can put together a custom-tailored program for both diagnosis and treatment.
Read More
Medical Minute: How to fit and use Crutches, Canes, and Walkers
How to fit and use Crutches, Canes, and Walkers
Welcome to another Medical Minute segment. Here, Haeleigh Little, a certified orthotic fitter from Colorado Springs Orthopaedic Group reviews how to properly fit and use crutches, canes, and walkers.
WHAT IS THE #1 THING PATIENTS STRUGGLE WITH WHEN FITTING WALKING ASSISTANCE DEVICES?
The number one thing patients struggle with is getting the height correct. The height for all of these devices will depend on body type. Most crutches will have markers that will allow for adjustments, but each body is different. Fit can change depending on each individual’s body length, leg length, and arm length.
WHAT HAPPENS IF ANY PIECE OF EQUIPMENT IS NOT FITTED PROPERLY?
If a piece of equipment is not fitted properly, then the ultimate concern is the risk of injury. If the crutch or cane is not properly fitted to a patient’s particular height, you risk injury to the shoulders, elbows, and wrists because you are now relying on those parts of the body to walk.
HOW TO FIT CRUTCHES
Typically, you will want your crutches to sit approximately two or three finger widths below the armpit. If the crutches are too short, you can risk putting excessive pressure on internal structures and muscles within the armpit. Next, you will want to ensure the crutch allows for a slight bend in the elbow, that way in the case of a fall, you do not hyperextend your arm, potentially causing injury.
HOW TO FIT CANES AND WALKERS
When fitting a cane, hold your arm down at your side, the top of the cane should hit at your wrist. You can do the same for measuring walkers, however you will want it to hit a bit above your wrist to compensate for slight bend your elbows as you walk with the device.
ANY OTHER TIPS?
The biggest tip we recommend for all patients to follow is: go slow, listen to your body, and be aware of your surroundings when using any form of walking assistance equipment.
HOW CAN SOMEONE SCHEDULE AN APPOINTMENT?
To schedule an appointment, please call the office at 719-632-7669. Colorado Springs Orthopaedic Group does require a prescription for walking assistance devices so you will want to make sure you have talked to either your orthopedic physician or family physician prior to scheduling your appointment.
With these tips, you can safely fit crutches, canes, and walkers, and be on the path toward healing.
Read More
Hip and Knee Replacement Testimonials
Hip and Knee Replacement Testimonials
Get back to doing the things you enjoy and find out if a hip or knee replacement is right for you with Colorado Springs Orthopaedic Physician, Dr. Tyler Bron. Dr. Bron specializes in complex hip and knee replacement surgery. He is one of the few surgeons in Colorado who uses the Mako Robotic Arm to assist in total knee replacements which allows him to be more precise in preparing existing bones and placing the implants.
Dr. Bron strives to be available to his patients to provide as much information as needed to ensure they are comfortable with any decisions made regarding treatment. As a general principle, he believes in conservative measures when appropriate and proceed to surgery only when necessary.
Dr. Bron believes that life is too short to live in pain and shares that “advances in surgical procedures for both hip and knee replacements can get you up on your feet and enjoying life”. Here are just a few of his patients and what they have to say about their experience.